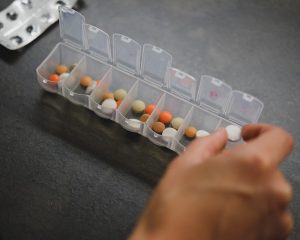
Significant evaluation metrics that should be part of the strategy.
This is the second installment of a two-part series based on key insights from a recent eHealth Initiative (eHI) panel webinar, “Using Evaluation Data to Drive Social Determinants of Health Program Improvement Strategies”. You can read Part One of our blog series here.
The Biggest Challenges When Designing SDOH Programs
Organizations often face difficulties with deploying robust evaluation strategies of their Social Determinants of Health (SDOH) interventions. Leaders can overcome this challenge by developing comprehensive evaluation plans at the start of the design of their intervention.
Leaders should choose evaluation metrics across multiple categories such as:
Individual metrics
Measure individual participant progress throughout the intervention:
- Quality of Life “Healthy Days”
- Clinical Indicators (e.g., Improving A1C)
- Surveys (e.g., Self-Efficacy, Customer Satisfaction)
- Number of addressed care gaps
- Reduction in risk levels and member acuity
- Stages of Change Theory related to specific health behavior or desired action (e.g., From Precontemplation to Action Stage)

Program operational metrics (e.g., number of referrals, number of individuals served)
Monitor the operational outputs of an intervention or program:
- Number of unique outreaches/attempts
- Number of successful connections
- Number of unique resource referrals
- Number of unique individuals served
- Number of unique individuals screened
- Number of completed risk screenings

Health outcomes (e.g., ambulatory care-sensitive condition emergency room visits, readmissions, cost of care)
Evaluate the impact of an intervention on a health outcome of interest:
- Readmission Rates
- Total Cost of Care
- Admissions
- ER visits
- Hospital acquired conditions
- Preventable Hospitalizations: Ambulatory Care Sensitive Emergency Department Visits
- Care Gaps Closed

Financial metrics (e.g., return on investment, cost avoidance)
Analyze the financial impact (i.e., savings and cost incurred) of an intervention:
- Return on investment
- Reduction in average length of stay
- Pre and post intervention Health care per member per month (PMPM) costs

Organizational impact metrics
Evaluate the downstream impacts of SDOH intervention on quality and patient experience measures:
- HEDIS measures
- Star ratings
- Access to healthcare
- Cultural competence
- Patient experience
Also, while defining metrics is an important component, program designers need to have a lens on the intervention and both when and where benefits will be observed. SDOH leaders often may face a “wrong pockets” issue. This is where one organization makes the large-scale initial investment or significantly supports the foundational infrastructure for the program, but another organization benefits from this investment.
This may occur a lot for colleagues working in children’s health where the ROI may come 5, 10, 15 years down the road. This can also help organizations focus on more complex populations that can benefit immediately from initiatives, categorizing them as high-cost and high-need, rather than spending time reducing risk for healthy populations.
What Do Healthcare Organizations Need to Keep in Mind?

In summary, panelists shared the following advice for healthcare leaders evaluating their SDOH programs:
- Healthcare organizations cannot tackle SDOH issues alone. Organizations should ask: is there a way to partner with other organizations that may benefit from the SDOH intervention to promote win-win scenarios? For example, can payers develop data-driven value-based arrangements with social service organizations?
- There are many ways to evaluate SDOH programs that are not directly measured by cost or dollars. Hospital systems need to remember that changing a patient’s overall health takes time and to define goals that are measurable, like the number of referrals accepted or even patient satisfaction. Don’t forget to work through the PDCA (Plan, Do, Check, Act) cycle to continuously move forward and iterate toward positive outcomes.
Resources That Support SDOH Evaluation
- Commonwealth ROI Calculator – This tool can help develop a ROI calculation based on SDOH interventions.
- The Transtheoretical Model (Stages of Change Theory) – The Stages of Change can be used as an evaluation measure to target the progress towards a desired health behavior action.
- Centers for Disease Control and Prevention (CDC) Healthy Days – Organizations can use this measurement to evaluate the impact of interventions.
- LexisNexis Socioeconomic Attributes, Scores, and Care Drivers – Socioeconomic data can help organizations in proactively enhancing care management activities and population health initiatives to improve health outcomes.
Want to see the archived panel discussion? Click here to access online.